Dysregulation of Serum Serotonin–Melatonin Biosynthetic Pathway Markers in Patients with Obsessive-Compulsive Disorder: A Case-Control Study
Downloads
Objective: Obsessive-compulsive disorder (OCD) is a disabling neuropsychiatric disorder associated with disturbances in neurotransmitter systems. This study aimed to investigate serum levels of serotonin, melatonin, and selected enzymes involved in their biosynthetic pathway in patients with OCD, and to determine the correlations among these biochemical markers.
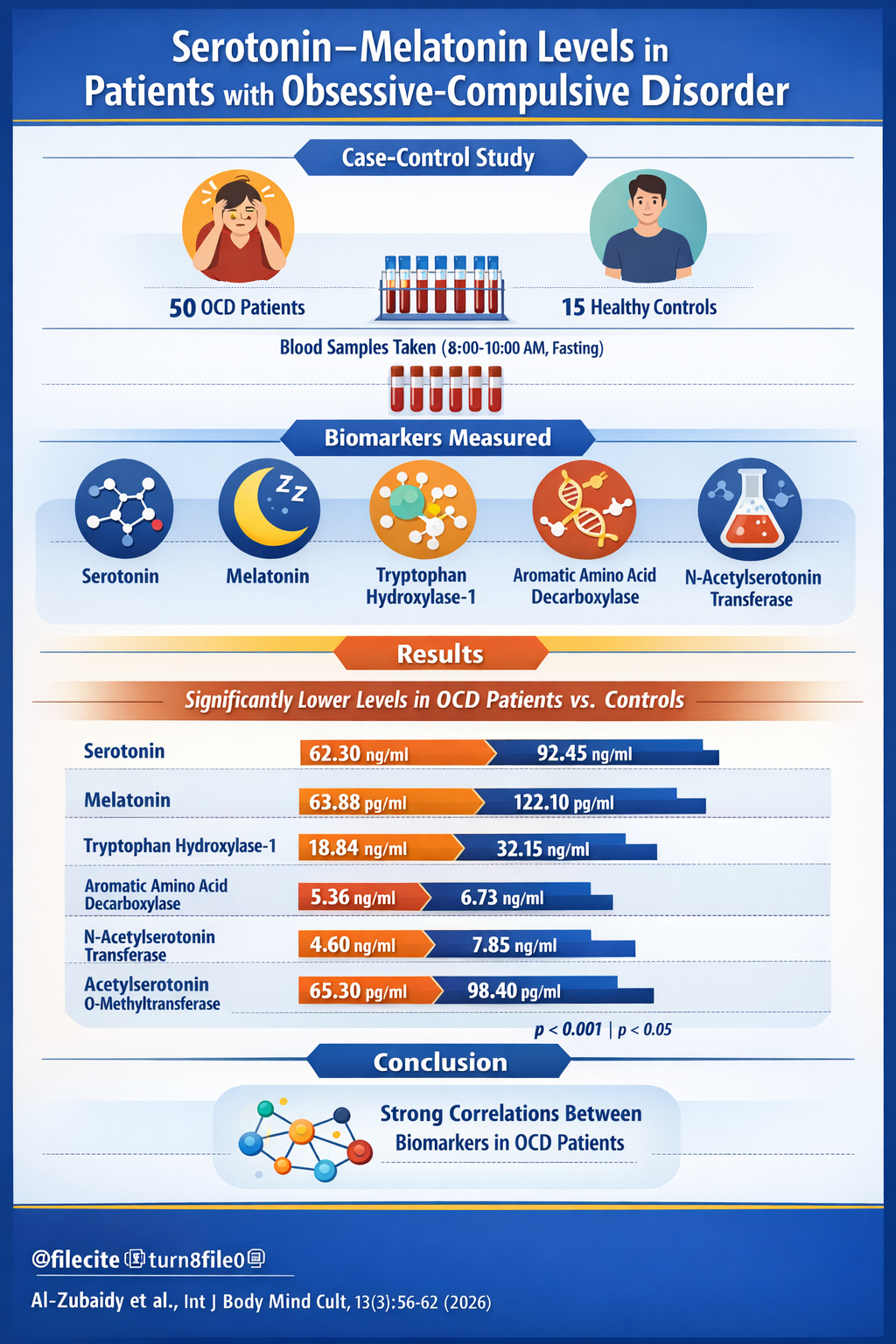
Methods and Materials: This case-control study included 50 patients with OCD diagnosed according to DSM-5 criteria and 15 age- and sex-matched healthy controls. Fasting venous blood samples were collected between 8:00 and 10:00 AM under controlled conditions. Serum concentrations of serotonin, melatonin, tryptophan hydroxylase-1 (TPH-1), aromatic amino acid decarboxylase (AADC), arylalkylamine N-acetyltransferase (AANAT), and acetylserotonin O-methyltransferase (ASMT) were measured using sandwich enzyme-linked immunosorbent assay (ELISA). Statistical analyses were conducted using SPSS version 26, with significance set at p < 0.05.
Findings: Serum levels of serotonin, melatonin, TPH-1, AANAT, and ASMT were significantly lower in patients with OCD than in healthy controls (all p < 0.001). AADC levels were also significantly reduced in the OCD group (p < 0.05). Furthermore, correlation analysis revealed significant positive associations among the studied biochemical parameters in patients with OCD, suggesting coordinated dysregulation within the serotonin–melatonin biosynthetic pathway.
Conclusion: Patients with OCD demonstrated significant reductions in serotonin, melatonin, and related biosynthetic enzymes. These findings support the possible involvement of altered serotonin–melatonin pathway activity in the pathophysiology of OCD and may provide a basis for future biomarker-oriented studies.
Downloads
Atmaca, M., Yildiz, S., Tabara, M. F., Gurok, M. G., Yildirim, M., & Yildirim, H. (2025). Reduced pineal gland volume in patients with obsessive-compulsive disorder. The International Journal of Psychiatry in Medicine, 60(5), 508-516. https://doi.org/10.1177/00912174241287996
Bear, M., Connors, B., & Paradiso, M. A. (2025). Neuroscience: Exploring the brain. Jones & Bartlett Learning. https://seti.net/Neuron%20Lab/NeuronReferences/Neuroscience%20-%20Bear.pdf
Catapano, F., Monteleone, P., Fuschino, A., Maj, M., & Kemali, D. (1992). Melatonin and cortisol secretion in patients with primary obsessive-compulsive disorder. Psychiatry Research, 44(3), 217–225. https://doi.org/10.1016/0165-1781(92)90025-X
De Deurwaerdère, P., & Di Giovanni, G. (2020). Serotonin in health and disease. International Journal of Molecular Sciences, 21(10), 3500. https://doi.org/10.3390/ijms21103500
Fatima-Shad, K. (2024). Serotonin-Neurotransmitter and Hormone of Brain, Bowels and Blood: Neurotransmitter and Hormone of Brain, Bowels and Blood. BoD–Books on Demand. https://doi.org/10.5772/intechopen.1000435
Goodman, W. K., Storch, E. A., & Sheth, S. A. (2021). Harmonizing the neurobiology and treatment of obsessive-compulsive disorder. American Journal of Psychiatry, 178(1), 17-29. https://doi.org/10.1176/appi.ajp.2020.20111601
Gutknecht, L., Araragi, N., Merker, S., Waider, J., Sommerlandt, F. M. J., Mlinar, B., Baccini, G., Mayer, U., Proft, F., & Hamon, M. (2012). Impacts of brain serotonin deficiency following Tph2 inactivation on development and raphe neuron serotonergic specification. PLoS ONE, 7(8), e43157. https://doi.org/10.1371/journal.pone.0043157
Hatamnejad, M. R., Baradaran Ghavami, S., Shirvani, M., Asghari Ahmadabad, M., Shahrokh, S., Farmani, M., Sherkat, G., Asadzadeh Aghdaei, H., & Zali, M. R. (2022). Selective serotonin reuptake inhibitors and inflammatory bowel disease: Beneficial or malpractice? Frontiers in Immunology, 13, 980189. https://doi.org/10.3389/fimmu.2022.980189
Jain, R., Chepke, C., Davis, L. L., McIntyre, R. S., & Raskind, M. A. (2024). Dysregulation of noradrenergic activity: Its role in conceptualizing and treating major depressive disorder, schizophrenia, agitation in Alzheimer’s disease, and posttraumatic stress disorder. The Journal of Clinical Psychiatry, 85(4), plunaro2417ah. https://doi.org/10.4088/JCP.plunaro2417ah
Keszthelyi, D., Troost, F. J., & Masclee, A. A. M. (2009). Understanding the role of tryptophan and serotonin metabolism in gastrointestinal function. Neurogastroenterology & Motility, 21(12), 1239–1249. https://doi.org/10.1111/j.1365-2982.2009.01370.x
Kurtuluş Dereli, A., Demirci, G. N., Dodurga, Y., Özbal, S., Cankurt, U., Boz, B., Adiguzel, E., & Acar, K. (2018). Evaluation of human pineal gland acetylserotonin O-methyltransferase immunoreactivity in suicide: A preliminary study. Medicine, Science and the Law, 58(4), 233–238. https://doi.org/10.1177/0025802418797178
Lv, Y., Li, Y., Li, J., Bian, C., Qin, C., & Shi, Q. (2020). A comparative genomics study on the molecular evolution of serotonin/melatonin biosynthesizing enzymes in vertebrates. Frontiers in Molecular Biosciences, 7, 11. https://doi.org/10.3389/fmolb.2020.00011
Michalowska, M., Znorko, B., Kamiński, T., Oksztulska-Kolanek, E., & Pawlak, D. (2015). New insights into tryptophan and its metabolites in the regulation of bone metabolism. Journal of Physiology and Pharmacology, 66(6), 779–791. https://ixcela.com/assets/uploads/research-studies/Tryptophan_BoneMetabolism.pdf
Nakamura, K., & Hasegawa, H. (2007). Developmental role of tryptophan hydroxylase in the nervous system. Molecular Neurobiology, 35(1), 45–54.. https://doi.org/10.1007/BF02700623
Pourhamzeh, M., Moravej, F. G., Arabi, M., Shahriari, E., Mehrabi, S., Ward, R., Ahadi, R., & Joghataei, M. T. (2022). The roles of serotonin in neuropsychiatric disorders. Cellular and Molecular Neurobiology, 42(6), 1671–1692. https://doi.org/10.1007/s10571-021-01064-9
Reiter, R. J. (1991). Pineal melatonin: Cell biology of its synthesis and of its physiological interactions. Endocrine Reviews, 12(2), 151–180. https://doi.org/10.1210/edrv-12-2-151
Shokrani, M., Askari, S., Eissazade, N., Shariat, S. V., Shariati, B., Yarahmadi, M., & Shalbafan, M. (2023). Agomelatine augmentation of sertraline in the treatment of moderate to severe obsessive-compulsive disorder: A randomized double-blinded placebo-controlled clinical trial. BMC Psychiatry, 23(1), 686. https://doi.org/10.1186/s12888-023-05189-7
Skorobogatov, K., De Picker, L., Verkerk, R., Coppens, V., Leboyer, M., Müller, N., & Morrens, M. (2021). Brain versus blood: A systematic review on the concordance between peripheral and central kynurenine pathway measures in psychiatric disorders. Frontiers in Immunology, 12, 716980. https://doi.org/10.3389/fimmu.2021.716980
Stahl, S. M. (2021). Stahl's Essential Psychopharmacology: Neuroscientific Basis and Practical Applications. Cambridge University Press. https://doi.org/10.1017/9781108975292
Stein, D. J., Costa, D. L. C., Lochner, C., Miguel, E. C., Reddy, Y. C. J., Shavitt, R. G., van den Heuvel, O. A., & Simpson, H. B. (2019). Obsessive-compulsive disorder. Nature Reviews Disease Primers, 5(1), 52. https://doi.org/10.1038/s41572-019-0102-3
van Dijk, A., Klompmakers, A., & Denys, D. (2008). Role of serotonin in obsessive-compulsive disorder. Future Neurology, 3(5), 589–603. https://doi.org/10.2217/14796708.3.5.589
van Oudheusden, L. J. B., van de Schoot, R., Hoogendoorn, A. W., van Oppen, P., Kaarsemaker, M., Meynen, G., & van Balkom, A. J. L. M. (2020). Classification of comorbidity in obsessive-compulsive disorder: A latent class analysis. Brain and Behavior, 10(7), e01641. https://doi.org/10.1002/brb3.1641
Wang, L., Chen, Y., Hu, S., Yu, T., Liu, Z., & Qiao, D. (2025). Influence of TPH2 DNA methylation and family functioning, parenting styles on OCD severity. BMC Psychiatry, 25, 882. https://doi.org/10.1186/s12888-025-07217-0
Copyright (c) 2026 International Journal of Body, Mind and Culture

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.















